Morton's Neuroma
What is it?
Moron's Neuroma, first described by Thomas Morton in 1876, is characterised as a pain in the forefoot caused by the entrapment of a nerve in the front of the foot by the metatarsal heads. The nerve becomes inflamed, swollen and painful.
"Neuroma" means nerve tumour (tumour in this case means simply enlargement of the nerve and not malignancy).
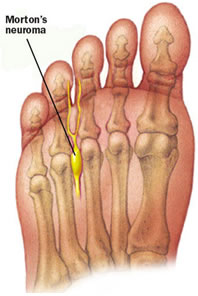
Symptoms
A Morton's Neuroma (interdigital neuroma) causes pain and numbness in the forefoot, usually between the 3rd and 4th toes. In some cases, the pain may also radiate out to the toes. It can also feel like cramp, pins and needles or electric shocks and settles after a few minutes once shoes are taen off. Classically, there is no pain when barefoot.
It is commonly mistaken with Metatarsalgia, another common cause of forefoot pain. The pain here is like walking on a pebble under the ball of the foot and used to be called a "dropped metatarsal". It is due to the joints becoming lax and inflamed. Importantly, the symptoms here are the opposite to a neuroma and it is often more comfortable in soft shoes, with increased pain when barefoot. It is especially painful standing on tiptoes or in high heels.
Mortons Neuroma and Metatarsalgia often occur together giving a mixed pattern of symptoms.
What causes it?
The cause is unknown but it is thought to be due to repeated squeezing and injury to the nerve, from wearing tight shoes. Each small injury causes the nerve to thicken slightly until the nerve becomes so big that it cannot fit between the metatarsals / toes.
Diagnosis
Diagnosis is usually straightforward and is based on the symptoms and careful clinical examination. Classically there is a positive Mulder's click – with pain when the nerve is squeezed between the metatarsals.
In complex cases, an MRi or ultrasound may be needed to confirm the diagnosis.
Treatment
- Wider shoes – have you shoe size checked and especially the width fitting.
- Custom insoles with a premetatarsal dome – this spreads the metatarsals out giving the nerve more room.
- Ultrasound guided injections of steroids. These can be very helpful but are often temporary.
- Surgery if the above measures fail. This is needed in approximately 2/3 cases.
“And do tell Mr Rosenfeld the foot has been perfect even on my walking holiday - no swelling, no pain, and i’ve been back doing sport on it for about 3 weeks now. I’m amazed how easy the recovery has been, and how effective the operation.”
Alison
Surgery
This involves carefully exposing the nerve and dividing it and removing it.
Click here for surgery information
Prognosis
v.good results if the diagnosis has been carefully made and confirmed. Recurrence in 5% of cases due to the cut nerve end forming a neuroma further back.
Surgery to remove a neuroma is successful around 90% of the time, however secondary complications may occur that necessitate further treatment. Occasionally there may be persisting pain due to the irritation of the cut end of the nerve, known as a stump neuroma. In some cases additional surgery is needed to remove this stump, if the pain does not desist. Additional problems with infection are also possible, but can be avoided with a good after care regime, as will be described by your specialist.