Peroneal Tendons
What are they?
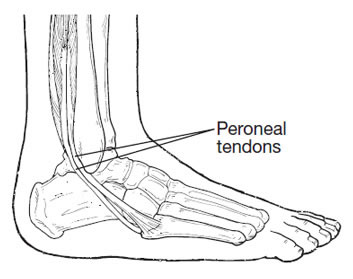 The
Peroneal Tendons are muscles (peroneus brevis and peroneus longus) that
form the outside part of the lower leg. These muscles are contained
within a sheath as they pass behind the out bone of the ankle joint,
before attaching to bones within the foot. They are responsible for
pulling the foot downwards and outwards. They also contribute to
stabilising the ankle joint.
The
Peroneal Tendons are muscles (peroneus brevis and peroneus longus) that
form the outside part of the lower leg. These muscles are contained
within a sheath as they pass behind the out bone of the ankle joint,
before attaching to bones within the foot. They are responsible for
pulling the foot downwards and outwards. They also contribute to
stabilising the ankle joint.
What causes damage?
The Peroneal tendons are usually damaged by any traumatic event, and are most commonly associated with an ankle sprain. However, there are some conditions that can lead to higher instances of Peroneal Tendon damage, such as rheumatoid arthritis, psoriasis, diabetes, a particularly high-arched foot (cavo-varus), or a complication from a steroid injection.
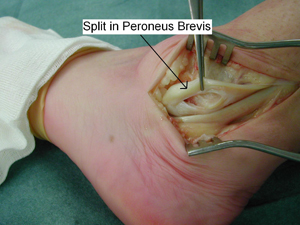
The form of the damage can take several forms, as with all tendon injuries. Repetitive trauma caused by overexertion may lead to tendon rupture, inflammation may lead to tendinosis or micro tears in in the tendon. Tendon injuries of this sort will cause pain along the outside of the ankle/foot, and may lead to weakness in the ankle, making it more likely that the ankle will give way on uneven ground, which can compound the damage. The sheath surrounding the tendons can also become damaged, allowing for the tendons to become dislocated around the fibula during ankle movement. This dislocation can lead to a painful 'clicking' sensation and ankle weakness.
Diagnosis
Most tendon injuries of this nature can be diagnosed by careful examination, with, with X-rays and MRI scans taken to determine if there is any traumatic or arthritic damage that may be contributing to the pain.
Treatment Options
Initial attempts to treat problems occurring with the peroneal tendons involve no-surgical interventions, designed to manage the discomfort with medication to reduce pain and inflammation. Temporary changes to lifestyle, such changing the footwear, reducing strenuous activity or temporary immobilisation may also help to alleviate the symptoms. Non-surgical techniques such as these often work for acute injuries and inflammations of the tendon sheath.
 The primary treatment options in order of escalation would be:
The primary treatment options in order of escalation would be:
- Physiotherapy
- Orthotics
- Steroids
- Surgery - rarely needed butusually successful
Prognosis
Surgical repair of the tendon has 80-90% good to excellent results, with most patients being able to return to previous levels of activity. Surgical repair of the sheath also has a high rate of full recovery, but in general will have a longer rehabilitation time before full functionality is restored. Post suregical complications are rare, but may include infection, recurrent injury, and damage to the sural nerve in the region.