Ankle Fusion (Open)
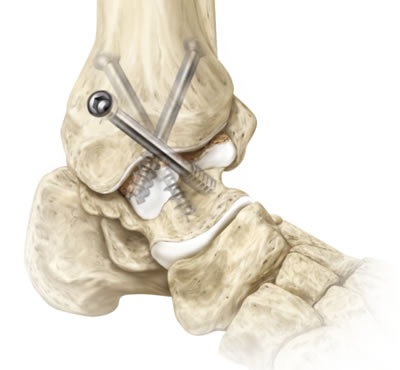
Age, or more often past injury, can cause arthritis affecting the bones of the ankle and the tissues that cushion and lubricate their articulation. This operation removes the degraded parts of the joints joint and fixes the joint together using metal screws and shaped plates - with the aim that bone will grow across and 'fuse' the joint. The joint will then be rigid, but no longer painful.
Also known as Ankle Arthrodesis, fusing the ankle reduces the normal range of movement by around 50%, although often the majority of this has been lost already, due to the arthritis. Walking will be altered, but not noticeably on flat ground. Walking on slopes and stairs is the most apparent difficulty and driving requires the use of the leg to push the pedals rather than by flexing at the ankle.
The surgery is performed through a 15cm incision over the outer side of the ankle. The arthritic joint surfaces are excised (cut out) and the joint fixed together with screws. The operation takes approximately 1.5 hours. After surgery, your leg will be immobilised in a backslab (half plaster) for 2 weeks.
Risks of surgery
Swelling
Initially the foot will be very swollen and needs elevating. The swelling will disperse over the following weeks & months but will still be apparent at 6-9 months.
Infection
This is the biggest risk with this type of surgery. You will be given intravenous antibiotics to prevent against it. The best way to reduce the chance of acquiring an infection is to keep the foot elevated for 14 days. If there is a mild infection, it often resolves with oral antibiotics. If the infection is severe, it may warrant admission to hospital and intravenous antibiotics. A severe infection often results in failure of the fusion, and extremely rarely may result in an amputation at a later date.
Malposition
Ideally, the ankle is fused in a position that allows optimum function and gives the best appearance. I take great efforts to judge the best position for the fusion at surgery, but as you are asleep and lying down, it is not al-ways possible to achieve this 'best' position. If the position is not optimal following surgery, most deformities can be accommodated by insoles and shoeware. Rarely is further surgery required.
Non Union
This is when the joint fails to fuse and bone has not grown across the joint. We won't know whether this is the case for 6-12 months. The risk of this is approximately 5%. Smoking increases this risk 4 times. If a non union does occur and is painful, then further surgery is usually needed.
Nerve Damage
Alongside the incision are two nerves – the superficial peroneal and the sural nerves. They supply sensation to the side and the top of the foot and toes. They may become damaged during the surgery and this will leave a patch of numbness, either at the side of the foot or over the top of the foot and toes. This numbness may be temporary or permanent. There is approximately a 10-15% of this happening.
"Dear Mr Rosenfeld
I was fortunate enough to have been the recipient of your expertise on February 24th of this year, 2017 at Charing Cross Hospital. I am writing to convey my infinite gratitude for what you did for me and to share with you the wonderful results of that operation. To say it has transformed my life doesn't even feel adequate so I shall have to revert to solid examples:
I live in a beautiful place, Marbella, I think we talked about that, and I am now able to walk the 10.7 kilometres to work up to 3 times a week appreciating and enjoying every step. Several friends have come to visit and it has given me enormous joy to be able to show them places such as Ronda and Granada on foot without needing to sit down and give up due to pain or seizing up as I used to call it. I feel no pain whatsoever in my ankle and I strongly believe that this has given me more confidence in every other part of my life too.To have a confident gait, a spring in one's step is a wonderful thing, far more valued after 16 years of not having had that.
Please, on my behalf, thank your wonderful team, especially Carlotta, who was always so kind and caring when I attended appointments at St. Mary's and again I cannot thank you enough for how wonderful it is to be able to walk properly and tell people to keep up with me instead of the other way round. Your eternally grateful ex-patient."
Jason A
Recovery from surgery
Elevation of the foot (above the pelvis) for the first 10 days is vitally important to prevent infection and reduce inflammation. Naturally, small periods of walking and standing are necessary, but no weight must be taken through this leg for 6 weeks.
After 2 weeks the backslab will be re-moved and the stitches taken out, here in clinic. Another non-weight bearing plaster is applied for a further 4 weeks.
At this stage you will be reviewed in clinic with x-rays and changed to a weight bearing plaster for a further 6 weeks.
You will be reviewed again at 3months following surgery, with x-rays. If all is well, no more plaster casts are needed and you can walk freely. Usually no physiotherapy is required. If the fusion has not completely healed, then a further 6 weeks in a weight bearing cast will be necessary.
Activity and time off work
As you will be wearing a plaster or plaster equivalent support for around 12 weeks, you may assume that recovery is a slow process that requires patience and care.
In general, 4 weeks off work is required for sedentary posts, 12 weeks for standing or walking posts, 16 weeks for manual / labour intensive posts.
Driving with a plaster is a particular problem and therefore presume that you will not be getting behind the wheel of a vehicle until you are free of these and can support your weight without pain.
Follow up
- 2 weeks for removal of sutures & Change Of Plaster
- 6 weeks in Foot & Ankle clinic - COP to WB cast / AP & Lateral X-rays
- 3 Months for Removal of POP / Xray Ankle WB AP & Lateral X-ray / Mobilise FWB out of POP
- 6 months for final assessment if no complications